If you’re unsure about what you need to do to prepare for Florida’s Agency for Health Care Administration (AHCA) EVV mandate, you’re not alone.
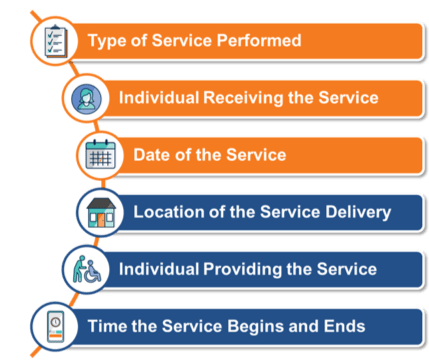
While Electronic Visit Verification (EVV) has been around for more than twenty years, with the passing of the 21st Century CURES Act, EVV is now a requirement for Medicaid homecare providers. The CURES Act requires homecare visits to be electronically verified for the type, date, and location of the service being performed; the individual receiving the service; the caregiver or aide performing the service, and the time the service begins and ends.
HHAeXchange is the industry leader in providing EVV solutions across the country with over 198 million visits confirmed annually through our platform, and we are actively providing solutions to meet EVV requirements for Florida homecare agencies. Check out all of the details below to get up to speed on what’s happening in the Sunshine State.
When is Florida’s EVV deadline?
AHCA has directed SMCC health plans to require providers to electronically verify visits for all home health and personal care services starting December 1, 2019.
UPDATE (3/27/2020): Due to the COVID-19 pandemic, the Medicaid health plans will not require providers to submit claims through the EVV system. Providers can continue to submit claims through the EVV system if they wish, but are not required to do so. Providers must, however, continue to verify the delivery of services (checking in at the start of a visit and checking out at its conclusion) using EVV technology, to the fullest extent possible.
What’s required?
The SMCC health plans must ensure that at least 85% of all visits paid will be verified using EVV and has established monthly targets for compliance. AHCA issued these targets as well as the provider guidelines below in a notice sent on January 31st, stating that:
-
Providers utilize the MCOs’ EVV system and a valid EVV method.
-
Providers are required to provide a valid exception reason (override) for visits not submitted with a valid EVV method.
-
Providers must report any technical difficulties with the MCOs’ EVV system to the EVV vendor and the MCO.
You can read more in the notice sent by AHCA on January 31st.
Whom does this impact?
EVV is required for all home health services including home health visits, private duty nursing, and personal care services. According to AHCA, providers must:
• Verify delivery of services using an EVV system at the beginning and end of each home health service visit.
• Submit claims through the vendor’s system to verify that delivered services comply with prior authorizations before claims can be processed for payment.
What is the status of EVV in Florida?
Florida is an Open Model state. This means providers are free to choose any EVV solution that best meets the needs of their agency. The only requirement is that the selected EVV solution must collect all six data elements as required by the CURES Act.
What if I’m connected with an MCO?
If you’re contracted with one of the MCO’s, you can continue to use your current EVV solution, as long as your vendor can send the correct information to the MCO’s visit confirmation and claims platform.
We recommend checking with each of your payers to confirm their individual deadlines for submission of visits and claims through their selected vendor.
If you’re contracted with Humana, Molina, Staywell, or Sunshine Health – you’ll submit your visit confirmations and send claims through the HHAeXchange Platform. Visit the HHAeXchange Provider Info Center for more details, dates, training sessions, and resources.
What about the state’s aggregator?
AHCA has contracted with Centric Consulting, LLC (Tellus) to aggregate EVV data on behalf of the State. However, you do not need to directly contract with the State’s aggregator. There is no charge to your agency to send EVV data to the State, and in many cases, your EVV platform, including HHAeXchange, will send this data to the State’s aggregator on your behalf.
What are the penalties?
If a provider fails to comply with these rules, they are subject to denial or non-payment of claims, sanctions, fines and suspension, or termination, from the Florida Medicaid program according to Rule 59G-9.070 Administrative Sanctions on Providers, Entities and Persons.
What are my next steps?
Since Florida is an Open Model state, providers are free to choose the EVV solution that best meets the needs of their agency and complies with the CURES Act requirements. However, make sure that your selected solution can transmit data electronically to both the MCO’s vendors and the State’s Aggregator.
Want to learn more about EVV in Florida? Contact us today.
This post was updated on Thu Oct 16 2025.

